The human papillomavirus (HPV) is a very common sexually transmitted infection worldwide.
The peculiarity of this infection is that it may not manifest itself for many years, but eventually leads to the development of benign (papilloma) or malignant (cervical cancer) diseases of the genital organs.
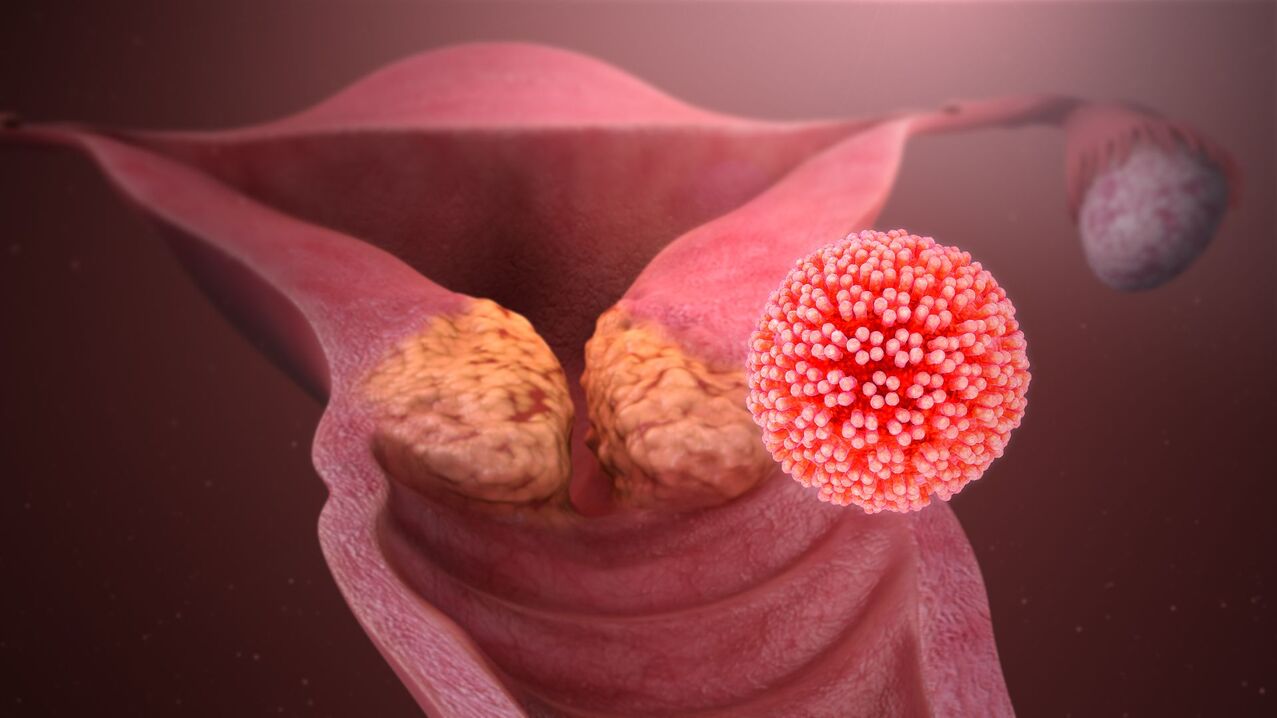
Types of human papillomavirus
More than 100 HPV types are known. Types are special "subtypes" of a virus that differ from one another. Types are identified by numbers assigned to them when they were discovered.
The high oncogenic risk group consists of 14 types: 16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 66, 68 (these types are associated with the development of cervical cancer).
In addition, types with a low oncogenic risk are known (mainly 6 and 11). They lead to the formation of anogenital warts (genital warts, papillomas). Papillomas are located on the mucous membrane of the vulva, vagina, in the perianal area, on the skin of the genital organs. They almost never become malignant, but lead to significant cosmetic defects in the genital area. Warts on other parts of the body (hands, feet, face) can also be caused by these types of viruses or have a different origin. In the following articles, we will discuss the high-risk and low-risk HPV types separately.
Human papillomavirus infection
The virus is mainly transmitted through sexual contact. Almost all women will sooner or later become infected with HPV: up to 90% of sexually active women will experience this infection at some point in their lives.
But there is good news: the majority of those infected (about 90%) get rid of HPV within two years without medical intervention.
This is the normal course of the infection process in the human body caused by HPV. This time is enough for the human immune system to completely get rid of the virus. In such a situation, HPV will not harm the body.That is, if HPV was detected some time ago and now it is not, this is absolutely normal!
It must be borne in mind that the immune system works at "different speeds" in different people. In this regard, the speed of getting rid of HPV can be different for sexual partners. Therefore, a situation is possible where HPV is in one of the partners, and not in that oneis recognized by others.
Most people become infected with HPV shortly after becoming sexually active, and many will never know they have been infected with HPV. No permanent immunity is formed after infection, therefore it is possible to become infected again both with the same virus that one has already encountered and with other types of viruses.
"High-risk" HPV is dangerous because it can lead to the development of cervical cancer and some other cancers. "High-risk" HPV causes no other problems.
HPV does not lead to the development of inflammation of the lining of the vagina/cervix, menstrual irregularities, or infertility.
HPV does not affect the ability to conceive and carry a pregnancy.
A "high-risk" HPV baby is not transmitted during pregnancy and delivery.
Human papillomavirus diagnosis
It is practically pointless to have an HPV test for high oncogenic risk before the age of 25 (except in women who start sexual activity early (before 18 years of age)), because at that time a virus is very likely to be detected thatsoon occur the body is left to its own devices.
After 25 - 30 years, an analysis makes sense:
- together with a cytological analysis (PAP - test). If there are changes in the PAP test and HPV "high risk", then this situation requires special attention;
- The long-term persistence of "high-risk" HPV without cytological changes also deserves attention. It has recently been shown that the sensitivity of the HPV test in the prevention of cervical cancer is higher than the sensitivity of cytology, and therefore the determination of HPV alone (withoutcytology) approved as a standalone study for the prevention of cervical cancer in the US However, annual cytology is recommended in our country, so a combination of these two studies makes sense;
- after treatment of dysplasia / precancer / cervical cancer (absence of HPV in post-treatment analysis almost always indicates successful treatment).
For the examination it is necessary to obtain a smear from the cervical canal (it is possible to examine the material from the vagina, but it is recommended to take the material from the cervix as part of the screening).
The analysis must be given:
- 1 time per year (if high-risk HPV was previously detected and the analysis is carried out together with a cytological examination);
- 1 time in 5 years if the previous analysis was negative.
Analysis for low oncogenic risk HPV is almost never required. If there are no papillomas, this analysis is basically not useful (virus transmission possible, virus treatment not possible, further procedure with the analysis result is therefore unknown).
If there are papillomas, then:
- most commonly they are caused by HPV;
- they must be deleted whether or not we find 6/11 types;
- When we take a smear, it is directly from the papillomas themselves, and not from the vagina / cervix.
There are tests to detect different types of HPV. If you are regularly tested for HPV, be aware of which specific types are included in the analysis. Some labs only research types 16 and 18, others all types together. It is also possible to run a test that identifies all 14 types of "high-risk" viruses in a quantitative format. Quantitative characteristics are important in predicting the likelihood of developing precancerous lesions and cervical cancer. These tests should be used in the context of cervical cancer preventionand not used as a stand-alone test An analysis for HPV without cytology results (PAP test) usually does not allow any conclusions to be drawn about the patient's state of health.
There is no such analysis that determines whether or not the virus "goes away" in a given patient.
Treatment of human papillomavirus
There is no medical treatment for HPV. There are treatments for diseases caused by HPV (papilloma, dysplasia, precancerous lesions, cervical cancer).
This treatment should be carried out using surgical methods (cryocoagulation, laser, radio knife).
No "immunostimulants" are related to the treatment of HPV and should not be used. None of the drugs that are widely known in our country have passed adequate tests that would show their effectiveness and safety. None of the protocols/standard/recommendations include these drugs.
The presence or absence of "erosion" of the cervix does not affect the tactics of HPV treatment. You can read more about situations where erosion needs to be treated in the article Erosion or not Erosion? " read up.
If the patient has no complaints and there are no papillomas / changes on the cervix during colposcopy and according to the PAP test, then no medical intervention is required.
It is only necessary to repeat the analysis once a year and control the condition of the cervix (annually PAP test, colposcopy). In most patients, the virus "exits" the body on its own. If it does not go away, it is not at all necessary that it leads to the development of cervical cancer, but control is necessary.
Treatment of sexual partners is not required (except in cases when both partners have genital papillomas).
Prevention of human papillomavirus infection
Vaccines have been developed that protect against HPV types 16 and 18 (one of the vaccines also protects against types 6 and 11). HPV types 16 and 18 are responsible for 70% of cervical cancer cases, which is why protection against them is so important. Routine vaccinations are carried out in 45 countries around the world.
Condom (does not provide 100% protection).
The only method that offers 100 percent protection is not to have sex. I'm not promoting him in any way, just food for thought.














































































